Travelers Diarrhea ~ Symptoms ~ Treatments ~ & When to Call the Doctor
Never pleasant, travelers diarrhea is the most common illness affecting travelers ~ in fact, 40% to 60% of people travelling from developed to developing areas will contact some form of travellers diarrhea, according to the Journal of Travel Medicine. Most of the time travelers’ diarrhea is not severe and will resolve on its own within 4 days. However, severe cases may lead to travel schedule changes, doctor’s visits, and even serious dehydration which can have dangerous consequences if it is not addressed by a healthcare professional.
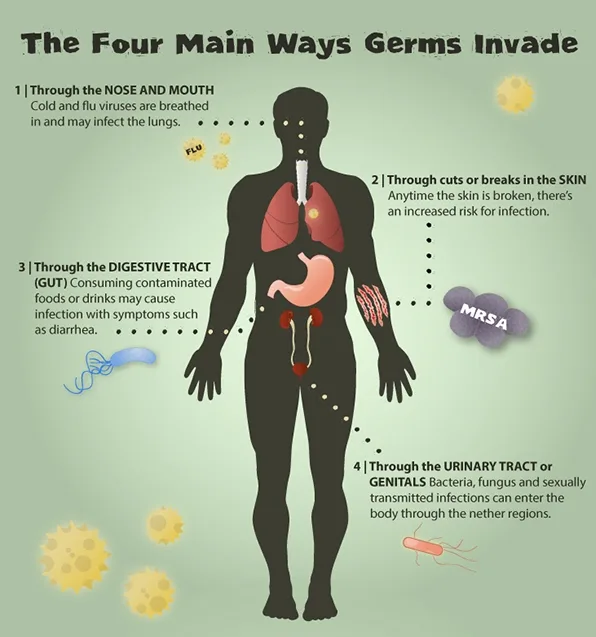
Causes
Bacterial, viral, or parasitic infections can cause travelers’ diarrhea. Most commonly, the infection is caused by E. coli bacteria. The microbes that causing this type of infection can be found in contaminated food and water.
If you have a weakened immune system, diabetes, an inflammatory bowel disease like crohn’s or ulcerative colitis, cirrhosis, or take antacids for peptic ulcer disease or heartburn, you have increased chances of contracting travelers’ diarrhea.
Classification System for Traveler’s Diarrhea according to the the International Society of Travel Medicine:
Mild ~ Diarrhea that is tolerable, not distressing, and does not interfere with planned activities
Moderate ~ Diarrhea that is distressing or interferes with planned activities
Severe ~ Diarrhea that is incapacitating or completely prevents planned activities; all dysentery (passage of bloody stools) is considered severe
Signs and Symptoms
- Watery diarrhea (three or more stools per day)
- Urgency (feeling like you need to use the bathroom NOW)
- Malaise (general achy, tired feeling)
- Decreased appetite
- Abdominal cramping
- Possible nausea or vomiting and/or low fever
When to Call the Doctor
Some types of traveler’s diarrhea are more serious and severe ~ we suggest you seek medical help if you have any of the following:
- Moderate/ Severe diarrhea as mentioned above
- If you are uncomfortable and it is interfering with your travel plans
- Fever
- Uncomfortable ~ abdominal pain or cramping
- Bloody diarrhea
- Mucus in diarrhea
- Vomiting that persists past the first day
- Signs and symptoms of dehydration (dry mouth, being hot but not sweating, decreased urination, dark urine, mental changes)
- Tenesmus (feeling like you frequently need to use the bathroom even when your bowels do not need to be moved)
- If you have taken antibiotics in the past few months and have had upper gastrointestinal problems (bloating, flatulence (gas), cramping) or diarrhea following the antibiotic use please notify your doctor
- Diarrhea that has not resolved on its own in 4 days
- signs and symptoms of colitis or upper gastrointestinal issues
- We also suggest you seek medical help if you have any other underlying health conditions that may put you at risk for additional complications~ examples may include heart or blood pressure issues etc.
- If you are a child, elderly, or have a weakened immune system
Be especially cautious with children & the elderly as traveler’s diarrhea can cause severe dehydration in a short time. Call a doctor if the patient exhibits any of the following signs or symptoms:
- Persistent vomiting
- Bloody stools or severe diarrhea
- A fever of 102 F (39 C) or more
- Dry mouth or crying without tears
- Signs of being unusually sleepy, drowsy or unresponsive
- Decreased volume of urine, including fewer wet diapers in infants
Treatment
According to the Australian Family Physician Journal, cases of traveler’s diarrhea usually get better within three to five days of fluid replacement.
In this case, replacing the fluid that your body loses from diarrhea is extremely important. People usually do not realize how dehydrated they can get from travelers’ diarrhea, especially in children and older adults.
- Drink lots of water and other clear liquids with glucose (sugar) and electrolytes like sodium chloride, potassium, and sodium bicarbonate. Sports drinks, broth, and juice are good choices.
- You can even make your own rehydration solution with a recipe from the World Health Organization Disease Control Programme:
Half teaspoon (3.5 g) of salt + 8 teaspoons (40 g) of sugar + 1 liter of water
- Stay out of the sun for long periods of time and make sure to take breaks to rest and rehydrate.
Over the counter antidiarrheal medication should be used with caution, always follow the directions and warnings on the label, and never take for a prolonged period of time.
Persistent diarrhea should always be treated by a doctor.
In this case, you may have a stool sample collected to determine what type of infection you have. After the cause is determined, the appropriate antibiotic medications may be prescribed. New research is showing that balancing your intestinal flora is an important part of good health and maintaining a healthy gut . Ask your doctor about probiotic treatment, to help replace the intestinal flora balance in conjunction with or following an antibiotic.
For more information on probiotics:
Prevention
Choose your Food & Drink Wisely: A list of foods and drinks that are usually safe:
- Fully cooked, hot foods (no raw or undercooked meat or seafood)
- Fruits peeled right before eating (bananas, oranges, or avocados, for example)
- Pasteurized dairy
- Bottled water and drinks
- Hot coffee and tea
Foods & Drinks to Avoid:
- Ice- freezing does not kill microorganisms like boiling does
- Improperly washed, room temperature salads (fruit, vegetable, chicken/egg, etc.)
- Buffet or street vendor food
Water Purification is another method of preventing travelers’ diarrhea. Methods include boiling (for 3 minutes then allowing the water to cool) and camping/wilderness water filters. In addition, don’t swim in contaminated water or allow contaminated water to go into your mouth. This includes when showering and brushing your teeth!
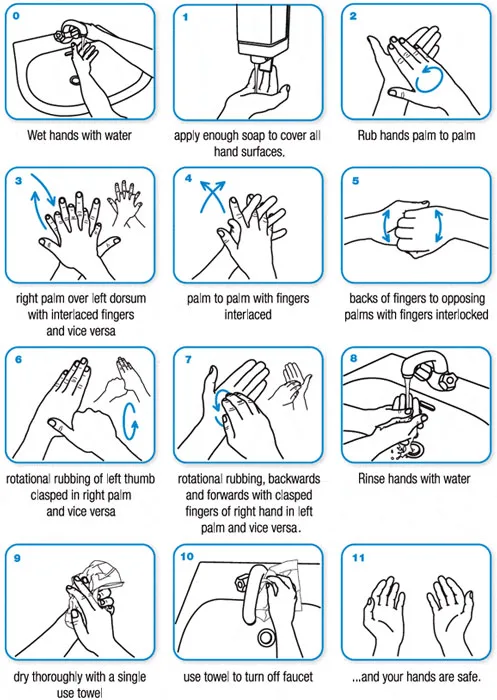
Handwashing is another great method for preventing travelers’ diarrhea. Are you always washing your hands the right way at the right times? Most likely not! Only 5% of people wash their hands correctly according to Michigan State University. Make sure you wash your hands for at least 20 seconds before eating and touching food, wounds, or your face and after making food, using the bathroom, touching animals, blowing your nose, coughing/sneezing, and touching garbage. In doubt, wash! When you cannot wash your hands, you should use alcohol hand sanitizer. Just make sure you use enough to completely cover your hands and allow it to dry.
Remember, MedinAction can provide your own personal doctor. Your visit will be private and confidential, in the comfort of your own home. Schedule an appointment with an English Speaking Doctor today. You can chat for free on our website, discuss your symptoms and decide if you require an appointment/ Treatment or just some free advice!
~ FREE Online Chat
~ Call/ Whatsapp or Text Message + 39 375 5724 686
~ MedinAction iOS app