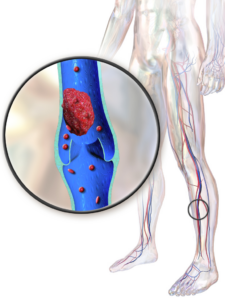
We’re now in peak travel season! Are you ready for your 8+ hour flight? What about that long car, bus, or train ride? The experience and destination are worth the hassle, but keep in mind the development of blood clots when embarking on long trips. According to the Centers for Disease Control and Prevention (CDC), anyone is at risk for a blood clot if they are traveling and sitting for more than 4 hours. In addition, there are certain factors that can increase your risk. So before you head out to the airport, take some time to read this article about blood clots and how to prevent them!
Blood Clots
Blood clots consist of platelets, red blood cells, and proteins that clump together when a blood vessel is damaged. This can be from injury, inflammation, or plaque buildup and rupture. However, blood clots can also form when there is no damage to a blood vessel. For example, you can have blood clots from sitting for an extended period of time due to a slow in blood flow. As a result, your platelets are more likely to clump together, leading to clot formation.
Two types of blood clots are thrombi and emboli. A thrombus is a blood clot that forms in one place and remains there. Once a thrombus breaks off and can travel, it is referred to as an embolus.
Blood clots can also be categorized by whether they originate in an artery or a vein. An arterial blood clot forms in an artery and can lead to a heart attack or stroke. A venous blood clot, the type discussed in this post, forms in a vein and does not cause a heart attack or stroke. However, a venous blood clot can cause a pulmonary embolism (discussed more in the next section).
Deep Vein Thrombosis (DVT)
Deep vein thromboses (DVTs) are a type of venous thromboembolism (VTE), blood clots that form in veins. DVTs are specifically located in the deep veins of your body. They usually occur in the legs but can also form around your pelvis, in you arms, and other spots as well. DVTs can have serious complications including disability and death. If this type of blood clot break off, it forms an embolism that can travel to other parts of the body, including the lungs. This is called a pulmonary embolism.
Even though your lungs breathe in oxygen, they cannot simply absorb it for themselves. Instead, they need their own blood supply like the other organs in your body. A pulmonary embolism is a blockage of an artery in the lungs. This means that the section of your lungs supplied by that artery does not receive the blood and oxygen it needs. If these lungs cells die, it’s harder for the lungs as a whole to do their job. Therefore, the rest of your body may not get enough oxygen.
But don’t panic. According to the CDC, most people have very little risk of developing DVTs and many times these clots can dissolve by themselves. Also, there are ways to prevent DVTs in the first place as well as effective treatments if they are discovered early.
Risks
In addition to the length of your travels, there are multiple factors that can increase your chances for DVTs:
- Personal and/or family history of blood clots
- Immobility
- Lack of movement can greatly increase your risk for DVTs due to slowed blood flow. This is true for anyone who is stationarily traveling for 4 or more hours, such as in a plane, car, or bus.
- See the “Prevention” section later in this post for ways to increase your movement when traveling!
- Surgery or injury
- Surgery and injuries like bone fractures and muscle injuries can damage veins, leading to blood clots.
- Cancer or chemotherapy treatment
- Pregnancy
- Estrogen-containing medications
- These include oral contraceptives and hormone replacement therapy
- Increasing age
- Risk increases once you are 40 or older. According to the American Heart Association, DVTs are most common in those over 60 years of age.
- Being overweight or obese
- Autoimmune disorders
- Blood marrow and/or clotting disorders
- If your bone marrow produces too many blood cells, your blood becomes thicker and clots more easily. Some blood clotting disorders also increase someone’s chances of DVTs due to changes in the structure and function of clotting proteins.
- Chronic diseases
- These include cardiovascular disease, lung disease, and inflammatory bowel disease.
- Smoking
If you have one or more of these risk factors, talk to your healthcare provider about preventative measures when traveling.
Signs and Symptoms
Around half of people with DVTs don’t experience any symptoms. If you do have signs and symptoms of a DVT, they are the result of the clot obstructing blood return to the heart:
- Swelling
- Pain (may be described as a throbbing or cramping)
- Tenderness
- Warmth
- Redness
You can look in the following picture at the patient’s right leg (the leg on your left, marked with the arrow). This individual’s leg is visibly swollen and red. If you touched his or her leg, it would most likely be warm. If you asked how it felt, he or she would most likely tell you that it was painful or tender.
The following are signs and symptoms of a pulmonary embolism (PE):
- Problems breathing
- Rapid heartbeat
- Chest pain (this may get worse when you cough or take a deep breath)
- Dizziness, lightheadedness, or fainting (indicative of low blood pressure)
- Coughing up blood
If you or someone else has symptoms of a DVT or PE, it is very important that you get medical attention right away. DVTs can lead to serious complications and PEs are life-threatening. Both of these conditions may be treatable with medications (anticoagulants or blood thinners, thrombin inhibitors, thrombolytic medications) and/or medical procedures (catheter-assisted thrombus removal, vena cava filter). However, every second is important!
Prevention
Although blood clots are serious and frightening, you can take action to help prevent them. When you are traveling, complete the following steps to reduce your risk of DVTs:
- Stand up and move around every 1 to 3 hours
- If you are on a bus or plane, try to pick an aisle seat so you can easily get up and walk around
- If you are in the car, take frequent breaks to stretch and move
- When walking around and stretching, try to do some calf raises, marching in place, quadriceps stretches, and forward folds/toe touches
- Do some stretches and light movement while in your chair. Here are some good examples:
- Toe-heel floor touches
- Keeping your heels on the floor- touch your toes to the floor, raise them up, and repeat 9 more times
- Keeping your toes on the floor- touch your heels to the floor, raise them up, and repeat 9 more times
- Muscle tightening and relaxing
- Contract (tighten) and release your leg muscles for a total of 5 times
- Ankle circles
- With your feet off of the floor, point your toes and move them in a circle. You can (1) move both feet clockwise then (2) counterclockwise; then (3) one clockwise and the other counterclockwise; then (4) switch. Repeat each of the four movements 4 more times.
- Knee lifts
- Bend your knees so your feet are flat on the floor. Lift one knee up so your thigh is off the seat. Lower that leg and switch sides. Repeat for a total of 10 times each leg.
- Toe-heel floor touches
- Avoid crossing your legs
- Stay hydrated
- Remember that drinking alcohol or caffeine can get you dehydrated. Drink plenty of water while traveling.
You may be asking why moving around is important in preventing blood clots.
Here’s the answer: When you move your legs, your muscles contract. These open up the valves in your veins to pump blood back to your heart, increasing blood flow and therefore reducing your risk of clotting.
If you have multiple risk factors for DVTs, make sure you talk with your healthcare provider. He or she may tell you to:
- Take medication that reduces your blood’s ability to clot, such as aspirin
- Wear compression stockings to improve blood circulation
- If you currently have a DVT, however, your healthcare provider may not recommend these for you. According to the United Kingdom’s National Health Service (NHS) and the American College of Chest Physicians, there has been conflicting evidence on the effectiveness of compression stockings in individuals with DVTs.
Just as you need your official passport for international trips, don’t forget to check out the National Blood Clot Alliance’s passport to safety to prevent blood clots when traveling!
Ask for an advice from an expert. Feel free to contact us!